
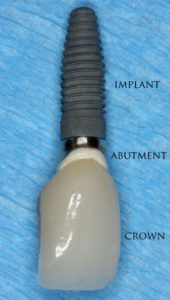
A dental implant used to replace missing teeth. The basis for modern dental implants is a biological process called osseointegration where materials, such as titanium, form a strong bond with bone. The implant fixture is first placed in the jaw bone. A variable amount of healing time is required for osseointegration before either the dental prosthetic (a tooth, bridge or denture) is attached to the implant or an abutment is placed which will hold a dental prosthetic.
 If you have the bone structure to support an implant, they are typically considered one of the most effective methods of replacing a lost tooth. Other benefits include:
If you have the bone structure to support an implant, they are typically considered one of the most effective methods of replacing a lost tooth. Other benefits include:
- Stronger and more comfortable than alternatives such as dentures or bridges
- Prevent bone loss in the jaw
- Minimal maintenance (brushing and flossing; same as natural teeth)
You might also consider getting implants if you’ve had a denture for many years but are looking for a non-removable alternative.
Coverage will vary between policies. Typically, dental insurance plans will offer minimal coverage for dental implants, but there are exceptions. We can confirm what is covered by your policy when you come in for an appointment or free consultation.





Hey, So Doc I have a underbite like barley noticeable and I am wondering if it’s a necessary to fix it like I was having to plan jaw surgery but then my orthodontist suggested something else an implant procedure which won’t correct it 100% but a little but my hygienist said I should do the surgery or I’ll have problems later on but my orthodontist said that people go through life without any problems with underbite so what do I do?
Hi Ismail, I understand this is a tough decision to make. I have many older patients with crossbite/underbite that don’t have any issues with their teeth. On the other hand, in some cases teeth are more likely to experience gum recession down the road due to underbite. I have also seen patients with severe underbite going through with the surgery and it being a life changing experience for them.
The surgery involves the sectioning of the lower jaw bones, re-positioning the jaw bones, and holding them in place with metal plates and screws. Braces are required both before and after the surgery to make sure the teeth are in the correct position after the surgery. The recovery period is long and difficult, and patients are typically on a liquid food diet and pain killers and not able to speak and work for a period of time. There is also a risk of nerve damage to the tongue, cheek, or lips, or damage to the roots of the teeth. For a surgery like this, you really have to look at the potential risks vs the benefits you expect to gain. If you’re still unsure, you can always seek a second opinion (from another orthodontist). Best of luck with your decision!
I’ve had several teeth either pulled or sanded down, completely improperly which has left me in an extremely uncomfortable state. What type of dentist should I see and what steps should I take to regrow the enamel on the sanded teeth and put back the teeth that are pulled, making sure they are alive in the process? I’ve been advised of artificial solutions before but per my research they will do even more damage so I will not consider them as an option, nor will I accept an answer that advises me to seek them, only one that will get me my original healthy teeth back. Thank you.
Hi Noah, unfortunately there is currently no commercially available treatment for regrowing enamel or teeth that have been extracted. There is research being done in this area though, so hopefully it’s an option dentists could offer in the future!
Hi I hope you can help me.
A year ago I had a tooth removed which left communication with the sinus. Last week I had a sinus lift using bone graft. Within five days the bone graft had fallen out of the hole where the communication had been. Im back to square 1. My question is, what was supposed to be holding the bone graft up stopping gravity just letting it fall out ? Because that’s pretty much just what it done. It just fell down into my mouth. 😕
Hi Tim,
For the sinus lift and bone graft you had, I am going to assume that you had particulate bone placed in. Particulate bone are loose smaller pieces of bone that can be more easily manipulated and packed into places. They are held in place by the sinus membrane on top, existing bone or gum on the surrounding surfaces, and gum facing the mouth is sutured together to prevent the grafting material from falling into the mouth. Sometimes a membrane maybe placed in between the bone graft material and the gum.
In some grafting cases, a larger single piece of bone or a block bone is needed if the bone defect is large. A block bone graft is usually held in place with mini screws. I hope this helps.
Hello. I have second molar moved into the position of first molar using TAD braces. I also now have an implant in the position where second molar used to be and I have to remove the implant or I can just bury the implant under the gums. Would I have to wear a retainer to prevent my second molar from tipping back where it used to be or would the buried implant prevent the movement of first molar?I can’t have more implants unfortunately
Hi Lizo, since the implant is not going to have a crown, it’s unlikely to prevent the crown of the original second molar from tipping back. Please follow the instructions of your orthodontist regarding the use of a retainer for your particular case.
Hello,
Two weeks ago I had the first stage of my front tooth implant done. Which the post was put in and a temporary tooth put on. For the procedure the dentist took some of my palette from the roof of my mouth, and stitched it to my front new post tooth gum line. So now I have stitches on the left side on the roof of my mouth, and my front right posted tooth gum line. Yesterday was the 2 week mark (march 23,2020 ) to remove my stitches, the dentist cancelled because of the corona virus, and rescheduled for April 20,2020. I am concerned that these none dissolving stitches and that this too long to be in. They did prescribed me a mouth wash. But still worried about the removal of the stitches. Can someone tell me what they think about my situation. Thank you.
Hi Sean, it will likely be perfectly fine to leave the stitches in for that period of time. Continue to brush and use mouth rinse as instructed by your dentist. The stitches may even become loose or come out on their own before your appointment, which is again perfectly fine. If you begin to experience increased pain, swelling, and/or pus coming from the grafting area, please contact an emergency dental office.
Because of COVID19 dentist appointments are canceled and I have braces and I was supposed to get them tightened you know routine but because I cant go will this affect my teeth or prolong the braces and should I still put on my elastics?
Hi Mike, followup appointments for orthodontic treatments are considered non-emergency dental treatments and are being rescheduled in most areas due to the COVID-19 pandemic. This should not affect your teeth negatively, but it may prolong the length of your treatment slightly depending on when you can be seen again. If your dentist or orthodontist prescribed elastics, please continue to wear them as instructed.
Greetings Dr. Li,
Thanks for this great Q&A service! For someone (me!) whose crown on tooth #3 fell out leaving a hopeless tooth at gumline that needs extraction, and next an implant, what is recommended timeline for getting fit for a nightguard needed for bruxism? Given significant expense of quality nightguards, I don’t want to have impressions taken before extraction if Im just going to need a new appliance 6 months later at time of implant bc of any mouth changes (bite shifting, bone loss, etc.) that might occur in interim. What would you advise – or maybe if you cant answer directly about my situation, what are general treatment recommendations for this type of scenario? Does the dental science tell us anything about best timing strategies for folks like me?
Thanks again for your time and for sharing your expertise!
Hi Casey, a custom made night guard is usually recommended after the crown is fitted on the implant. It will help to protect the implant from the effect of bruxism.
While you are in the extraction and implant stage for an upper molar tooth, there are a few options depending on your budget and how bad the bruxism is. Your dentist may be able to do an interim (thinner and cheaper) night guard for the upper teeth while things are healing. You can also ask your dentist for a recommendation for a Do it yourself night guard kit that you can purchase from a pharmacy for the upper teeth while things are healing. If those two options are not for you, and you need a custom made night guard before your upper implant crown can be completed, your dentist could make a lower night guard which will require minimal bite adjustment once your upper implant crown is finished.